Post-operative chronic pain is of growing concern after hernia repair with mesh. Though causes of pain may vary from patient to patient, one main aspect of pain is the inflammation associated with the use of most implanted surgical mesh. While mesh design technology has advanced through the years, the most widely used mesh products for hernia repair remains synthetic materials, typically polypropylene. These have been shown to be the best product for long-term durability of the repair.
In the U.S., over a million hernia repairs are performed annually, with about 350,000 ventral hernia repairs and 750,000 inguinal hernia repairs performed each year.i,ii These are common, sometimes challenging, procedures that are performed by general surgeons, plastic reconstructive surgeons, and some urologists and pediatric surgeons. Mesh implantation is considered the standard of care to reinforce soft tissue and help prevent hernia recurrence.
Nationally, we know that up to 20 percent of patients will have post-operative pain that lasts beyond the first 3 months of their hernia operation, the definition of chronic pain.iii This is much higher than the risk of hernia recurrence, which is typically well under 10 percent.iv The use of synthetic mesh has contributed to the low risk of hernia recurrences. Now, we must focus on improving quality of life after hernia repair by seeking mesh design to help reduce the incidence of chronic pain.v
In my practice, 80 percent of the patients referred to me have already suffered a complication from hernia repair. Half of these patients have chronic pain associated with their repair, which I see more often after inguinal hernia repair than after abdominal or ventral hernia repairs. The pain can be debilitating, leading to loss of work, depression, and even loss of one’s support system.vi This phenomenon of chronic post-operative pain has also contributed to our national epidemic of opioid abuse.
Some of the initial pain, swelling, and even bloating associated with hernia repair can be attributed to the inflammatory potential of the implanted surgical mesh. Macrophages, T-cells and mast cells each play a role the body’s inflammatory response and tend to proliferate when a foreign material is present.vii This usually resolves, though in some patients, the inflammation does not resolve and may be transmitted to nearby structures, such as nerves and the spermatic cord. In these patients, their pain may be chronic and unrelenting.
This adverse reaction seems to be more common after open inguinal hernia repair. There is something about the groin and pelvis region that does not tolerate the mesh implant as well as the rest of the abdomen. A subset of patients has been shown to be more prone to post-operative chronic pain than others. These include younger, underweight patients, whereas chronic pain is less likely among the elderly.viii Women have been shown to experience post-operative pain after inguinal hernia repair with mesh more often than men; both may suffer an impact on their sexual function and fertility. Those with inflammatory or autoimmune disorders may be at higher risk for mesh-related chronic pain. These include patients with lupus, rheumatoid arthritis, and fibromyalgia. As a result, multiple patient lawsuits have been filed related to synthetic mesh insertion in the groin and pelvis and its systemic and local complications.
Dr. Shirin Towfigh estimates 80 percent of the patients referred to her at the Beverly Hills Hernia Center in Los Angeles have already suffered a complication from hernia repair.
Today, the surgeon has a choice between synthetic and biologic mesh products for implantation. Synthetic mesh serves as a permanent barrier and provides a long-lasting scaffold onto which the patient’s tissue can adhese or grow. The method of ingrowth is typically triggered by the patient’s own inflammatory process against the mesh product. Synthetic mesh is durable; however, it typically does not stretch, and even contracts, resulting in stiffness and pain. Future operations in the area can become complicated and also place the mesh at risk for infection. Almost all synthetic mesh is made of pro-inflammatory materials including polypropylene or polyester fibers. It is the main method of its successful performance. In fact, synthetic mesh products treated with barriers that reduce their inflammatory potential have shown poor results, such as poor integration into the patient’s tissue and chronic seroma formation.
Biologic mesh is derived from tissue, including intestine or skin that has been processed and disinfected for use as an implanted device. The tissue is sourced from pigs, cows, sheep or humans. Biologic mesh serves as a resorbable scaffold for cellular repopulation with eventual remodeling into a patient’s tissue. The quality of this remodeled tissue can vary from patient to patient and is very product-dependent. This can lead to mixed clinical results. The main benefit of pure biologic tissue is that no foreign body is implanted in the patient to contribute to prolonged inflammation. Biologic mesh, however, is expensive and clinical results have not yet proven its equivalence to synthetic mesh in terms of long-term durability.
A newer category of long-term absorbable synthetic mesh was introduced to the market in 2011. Since then, a few products have been developed which are slightly less expensive than biologic tissue. Examples of absorbable synthetics include Poly-4-hydroxybutyrate, lactide and trimethylene carbonate.ix,x,xi They tend to begin absorption at about six months, and they are fully absorbed at up to 18 months. The consideration is that if the mesh product absorbs slower and over a longer period of time than biologic mesh, it is more beneficial. Studies to date have not conclusively shown that long-term absorbable synthetic mesh is equivalent to non-absorbable synthetic mesh. Long-term data is still pending for some products.
There are limited options for patients who are most at risk for adverse reactions to synthetic mesh and yet would benefit from long-term durability from a hernia repair. Our field still requires advancements in technology for soft tissue repair with the aim of minimizing the amount of foreign body used to achieve this. Fortunately, as chronic pain and foreign body reaction have become central issues in the treatment of hernias, this area has become one of rapid innovation.
In particular, the prospects of new hybrid materials that are emerging are very exciting. The goal of a hybrid mesh is to combine the best qualities of both synthetic and biologic mesh while reducing the drawbacks from each material. Mesh that combines biologic building blocks derived from animal tissue with a small amount of synthetic material, such as polypropylene, has the potential to reduce the risk of inflammatory reactions while still providing adequate long-term durability.
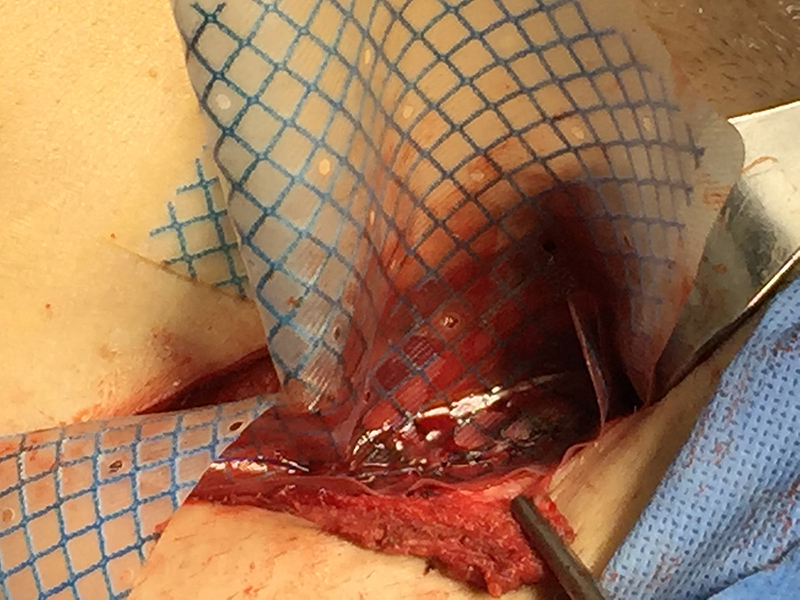
Hybrid surgical mesh for hernia repair combines synthetic and biologic materials, potentially reducing the risk of inflammatory reactions while still providing adequate durability.
The first hybrid mesh reached the market in 2014, and another promising hybrid mesh has launched this year.xii The biologic component of the mesh is the primary form of short-term treatment of the hernia. It provides a strong scaffold and barrier, equivalent to most synthetic mesh. As a hybrid mesh, a limited amount of synthetic product is integrated into the biologic tissue. Once the biologic tissue is resorbed, the synthetic component remains. However, unlike acutely implanted synthetic mesh, there is less inflammatory response expected from the hybrid mesh. That is because the synthetic mesh is already integrated into the repair as the biologic is resorbing. Also, there is significantly less synthetic mesh in the hybrid mesh counterpart, as the biologic tissue augments the early strength of the repair.
The goal is to provide the best surgical outcome without hurting the patient. With this goal in mind, the medical device industry must support continued research and education to advance the integration of synthetic and biologic materials in the development of the ideal mesh product. This type of innovation might have a broader impact beyond hernia repair. The use of surgical mesh in breast reconstruction is increasing, especially in cancer patients who have undergone a mastectomy, and many of the same discussions about whether synthetic or biological materials produce the best outcomes still apply.xiii This is also true in orthopedic applications where mesh is used in trauma and reconstructive surgeries to reinforce soft tissue including ruptured tendons or torn ligaments.
At the same time, we need to learn more about why some patient populations are at higher risk for chronic pain, and how the inflammatory response can be modified to reduce that risk. For example, is it an issue or excess scar formation, nerve entrapment, neuroma formation, pressure, or inflammation from the mesh product itself, or is it the patient’s intrinsic response to the foreign body that needs to be modulated?xiv To date there is no pre-operative test to determine risk for a reaction to mesh implantation. We may need to approach this as a gender-specific problem, with potentially different designs and solutions for men versus women.
There is a path forward to address the rise of chronic pain following hernia repair. By improving technique, building surgeon experience, sharing best practices for pain reduction and identifying risk factors we can support better patient outcomes while the medical device industry works on new mesh options that combine the best elements of synthetic and biologic materials.
References
iSociety of American Gastrointestinal and Endoscopic Surgeons. Laparoscopic Ventral Hernia Repair Patient Information from SAGES. http://www.sages.org/publications/patient-information/patient-information-for-laparoscopic-ventral-hernia-repair-from-sages/.
iiThe Society for Surgery of the Alimentary Tract. SSAT Patient Care Guidelines: Surgical Repair of Groin Hernias. http://www.ssat.com/cgi-bin/hernia6.cgi.
iiiS.W. Nienhuijs, C. Rosman, L.J.A. Strobbe, A. Wolff, R.P. Bleichrodt, An overview of the features influencing pain after inguinal hernia repair, International Journal of Surgery, Volume 6, Issue 4, August 2008, Pages 351-356, ISSN 1743-9191, http://dx.doi.org/10.1016/j.ijsu.2008.02.005. (http://www.sciencedirect.com/science/article/pii/S1743919108000320)
ivFränneby U, Sandblom G, Nordin P, Nyrén O, Gunnarsson U. Risk Factors for Long-term Pain After Hernia Surgery. Annals of Surgery. 2006;244(2):212-219. doi:10.1097/01.sla.0000218081.53940.01.
vFerzli et al. Chronic Pain after Inguinal Herniorrhaphy. Journal of the American College of Surgeons. Vol. 205, No. 2, August 2007. ISSN 1072-7515. doi:10.1016/j.jamcollsurg.2007.02.081.
viFerzli et al. Chronic Pain after Inguinal Herniorrhaphy. Journal of the American College of Surgeons. Vol. 205, No. 2, August 2007. ISSN 1072-7515. doi:10.1016/j.jamcollsurg.2007.02.081.
viiRosch R, Junge K, Schachtrupp A, Klinge U, Klosterhalfen B, Schumpelick V. Mesh implants in hernia repair. Inflammatory cell response in a rat model. Eur Surg Res. 2003 May-Jun;35(3):161-6.
viiiNienhuijs, Simon Willem et al. Pain after Anterior Mesh Hernia Repair, Journal of the American College of Surgeons , Volume 200 , Issue 6 , 885 – 889. http://www.journalacs.org/article/S1072-7515(05)00108-0/abstract
ixVICRYL® (polyglactin 910) Woven Mesh & VICRYL® (polyglactin 910) Knitted Mesh. Ethicon US, LLC. http://www.ethicon.com/healthcare-professionals/products/hernia-repair-and-fixation/hernia-mesh-flat-mesh/vicryl-polyglactin-910-woven-mesh
xPhasix™ Mesh Fully Resorbable Scaffold for Hernia Repair. C. R. Bard, Inc. https://www.davol.com/sp/phasix-mesh/
xiTIGR® Matrix. Novus Scientific. http://novusscientific.com/row/products/tigr-matrix/technology/
xiiOviTex: Reinforced Bioscaffolds. TELA Bio. http://www.telabio.com/products.html
xiiiLogan Ellis et al. Biological and synthetic mesh use in breast reconstructive surgery: a literature review. World Journal of Surgical Oncology. April 21, 2016. doi:10.1186/s12957-016-0874-9.
xivFerzli et al. Chronic Pain after Inguinal Herniorrhaphy. Journal of the American College of Surgeons. Vol. 205, No. 2, August 2007. ISSN 1072-7515. doi:10.1016/j.jamcollsurg.2007.02.081.




